Options of Implant
Cataract Lens (IOL) Options — Find the Best Fit for Your Vision
Cataract surgery replaces your cloudy lens with a clear intraocular lens (IOL). Choices vary in range of vision, night halos, contrast, and spectacle independence. We select together—based on your eyes, lifestyle, and medical safety.

Monofocal
Sharp distance (or near) in one focal range; highest contrast; reading glasses usually needed.
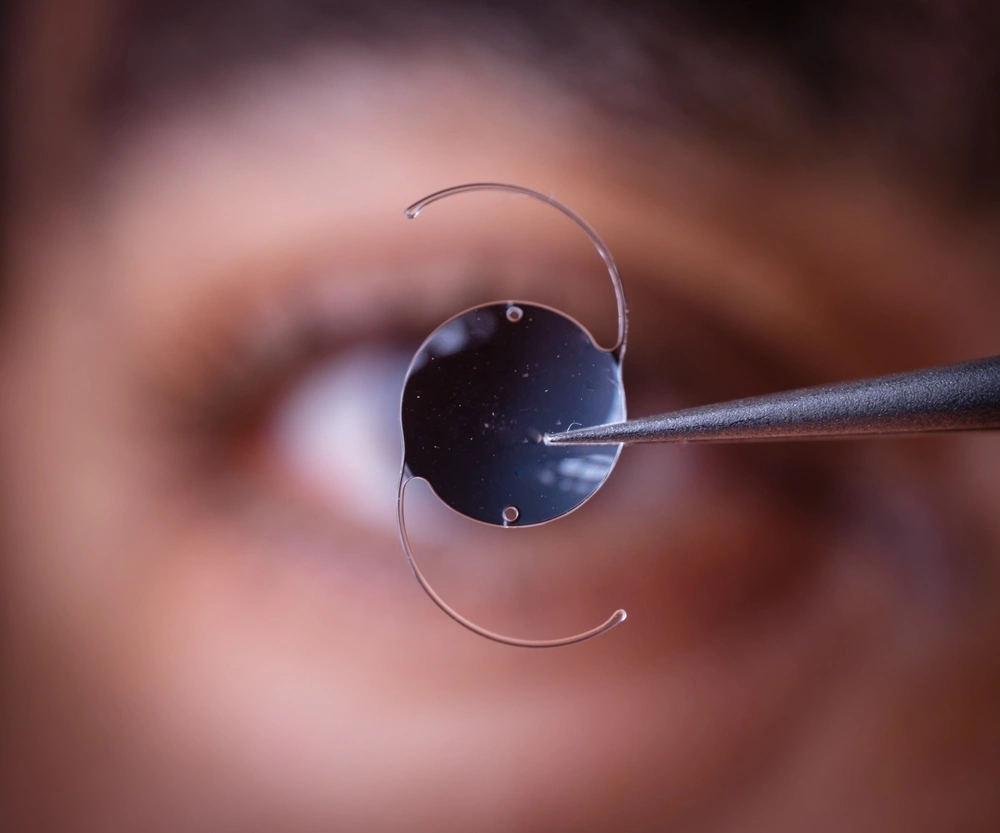
Advanced Monofocal (“enhanced”)
Similar safety/contrast to monofocal with better intermediate; some still need readers.

Toric (for astigmatism)
Any of the above with astigmatism correction; outcomes depend on rotation stability and precise alignment.

EDOF
Broader range to arm’s-length; fewer halos than trifocal but usually needs a light reader for fine print.

Trifocal
Distance + intermediate + near with highest spectacle independence; more halos/glare risk at night.
Book a cataract counseling session
Schedule your consultation with Dr. Praveen Saluja — begin your journey to clear vision.
Book an appointmentBook Cataract CounsellingFrequently Asked Questions
“Best” = what fits your cornea, macula, occupation, night driving, dry eye, etc. Evidence shows trade-offs (range of vision vs photic phenomena/contrast).
No—residual refractive error and neuroadaptation vary.
Toric IOLs — Cataract + Astigmatism Correction
- Corrects regular corneal astigmatism during cataract surgery. Outcomes depend on accurate axis alignment and post-op rotational stability.
- Follow-up focus: Early rotation checks improve outcomes; re-alignment can restore intended vision if misaligned.
Patients with ≥0.75–1.00 D corneal astigmatism.
Similar distance quality as monofocal when aligned; residual cylinder reduces sharpness.
Rotation, dry eye optimization, posterior capsular stability.
Marking/IOP control, capsulorhexis sizing, and modern guidance systems are used for precision.


Monofocal IOL — Gold-Standard Safety and Clarity
- Single focal point (usually distance); highest contrast and lowest night halos; readers usually needed.
- Ideal when macular disease, glaucoma risk, or night-driving priority. (Conservative choice remains evidence-supported.)
Excellent distance UCVA with refraction targeting.
Reading and sometimes computer glasses.
Ocular comorbidities, professional drivers, pilots, or halo-averse patients.
Advanced (Enhanced) Monofocal — Extra Range for Daily Life
- Preserves monofocal-like quality while boosting intermediate vision (dashboard/screen).
- Lower photic phenomena vs diffractive designs; many still need readers for fine print.
Office/computer users; halo-averse; early presbyopes.
Enhanced IOLs improve INT/Near vs conventional monofocals; more data emerging on contrast/QoV.


EDOF IOL — Wider Range, Natural Night Vision Profile
- Extends depth of focus for distance + intermediate and some near; typically fewer halos than trifocal but more than monofocal.
- Different platforms (diffractive vs refractive) show good distance, stronger intermediate, and variable near; contrast generally between monofocal and trifocal.
Professionals needing screens, active drivers at night, willing to use thin readers for fine print.
- Multiple 2024–2025 reports show better INT/near than enhanced monofocal and high satisfaction; residual Rx tolerance improving in newer refractive EDOF.
Trifocal IOL — Distance, Intermediate & Near with Max Spectacle Independence
- Highest chance of glasses-free across ranges; trade-off is more halos/glare and potential contrast reduction, especially in low light.
- Neuroadaptation usually improves symptoms over weeks to months. Comparative analyses show very high satisfaction despite more photic phenomena.
Strong desire for near independence, minimal ocular comorbidity, realistic night-driving expectations.
Pupil size, corneal quality, macular status, and dry eye optimization matter.


Trifocal IOL — Distance, Intermediate & Near with Max Spectacle Independence
- Day 1 (or within 24–48 hours): safety check (IOP, cornea, wound).
- Week 1: recovery on track, adjust drops, evaluate toric alignment if used.
- Week 3–6: dilated exam, final refraction, lifestyle fine-tuning; glasses if needed.
- Additional/virtual checks for selected low-risk cases may be appropriate per protocol.
- More frequent visits if ocular comorbidities or symptoms.

